Step into my time machine so we can travel back to 1989. We see you and your horse with the veterinarian examining the horse for lameness. Nerve blocks show the problem lies in your horse’s heels, but his X-rays look just fine. “He’s got navicular,” the vet says. “It’s just not bad enough to show up on X-rays yet.” It’s a devastating blow. You treat your horse with corrective shoeing and anti-inflammatories for years. You even inject his coffin joints. Unfortunately, he’s never really right, and his X-rays never change. “There must be something there,” you think. “I wish there was a way to look inside his feet and see what’s really wrong.”

Fast-forward a couple of decades. New horse, same problem. Your horse is lame, and nerve blocks confirm the pain is coming from his heels. “Not this again!” you think. “Isn’t there something more that we can do?”
Thanks to advances in imaging, yes! Here I’ll explain how advanced imaging options like nuclear scintigraphy (bone scan), magnetic resonance imaging (MRI), and computed tomography (CT) have changed the world of equine lameness diagnosis—especially involving your horse’s feet. You’ll see why nebulous answers like “navicular disease” or even “bilateral heel pain” have become obsolete, and how you can get an accurate and specific diagnosis instead. You’ll also learn how having a specific diagnosis can greatly improve your horse’s chances for a successful recovery.
Hoof Basics
Your horse’s foot is complicated. Add to that the many lameness problems that originate from the foot, and you’ll understand why it’s so important to be able to create accurate images of the area.
Thirty years ago, veterinarians focused most of their attention on the navicular bone—a small, wing-shaped bone in the back of the foot that distributes stress and assists the functioning of ligaments that both support your horse’s limbs on the ground and produce movement. If your horse was lame, a nerve block (deadening of the nerves that supply a certain area of the leg) might confirm the pain originates from his heels or foot. In the vast majority of cases, the navicular bone was blamed, and a diagnosis of “navicular disease” was made. Radiographs were taken. Sometimes the bone looked damaged; sometimes it didn’t. Sometimes your horse improved; sometimes he stayed lame for the rest of his life.
Now we know that those “navicular” horses likely had one of a wide variety of different, specific injuries, ranging from chronic degeneration of the bone itself to an acute injury of one of the many small tendons or ligaments within the foot. And through advances in technology, imaging techniques can identify specific injuries, which means that treatments can be more targeted and effective, and you’ll have a more accurate picture of your horse’s chances for recovery when a diagnosis is made.
IMAGING OPTIONS
Veterinary medicine has made major advancements since those years of diagnosing so many horses with navicular disease. These five imaging options play a large part in those enhancements to our diagnostic toolbox.
Radiographs
An X-ray machine passes a beam of radiation through your horse’s body toward a plate that detects the radiation, and then converts that information into an image to make a radiograph. Areas of the body that absorb more radiation appear white (thick bone), while areas that absorb less radiation appear dark (less thick bone or soft tissues). More modern systems (known as digital radiography or DR) are fully computerized, resulting in more detailed images that can be manipulated with a computer to help with interpretation.
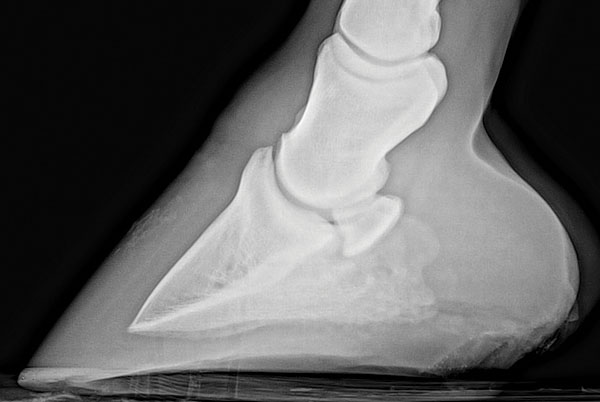
Pros: They provide a good overall assessment of the bones in your horse’s feet, including the navicular bone, and are especially useful for identifying fractures or bone degeneration. In some cases they show abnormalities where soft tissues attach. Comparing radiographs taken several years apart can show how significantly bones can change over time.
Cons: Radiographs don’t provide much information about soft tissues. Even when it comes to bone, radiographs are less sensitive than other imaging modalities such as MRI or CT. Studies have shown that there can be a great deal of bone inflammation present even though radiographs appear normal.
Ultrasound
The machine passes sound waves through your horse’s body parts to make an image. The waves are absorbed by or pass through tissues depending on tissue density, and a tiny microphone detects the waves that “bounce back” as echoes to develop and an image. Less-dense materials (like fluid) allow sound waves to pass completely through them and appear darker or “more black,” while dense tissues (like bone) will bounce back all of the waves and appear lighter or “more white.”
Pros: Ultrasound can provide accurate and detailed images of soft-tissue structures and joint surfaces. It’s especially useful to monitor healing of an injury throughout rehabilitation.
Cons: Accuracy depends on the operator’s skill. Ultrasound of the foot is particularly difficult to perform, in part because the hoof wall interferes with the passage of the sound waves. To get an accurate diagnosis, the ultrasonographer must be very experienced and have specialized equipment. And unlike other imaging modalities like radiography and MRI, images can’t be reliably sent to outside experts for review.
Magnetic Resonance Imaging (MRI)
MRI subjects a part of your horse’s body to a very strong magnetic field that impacts the alignment of tiny particles (called protons) within his cells. The magnetic field is manipulated using short bursts of radio waves that cause the protons to change their alignment. Protons in different types of tissues have characteristic responses, and send off unique signals that are detected and converted to an image.
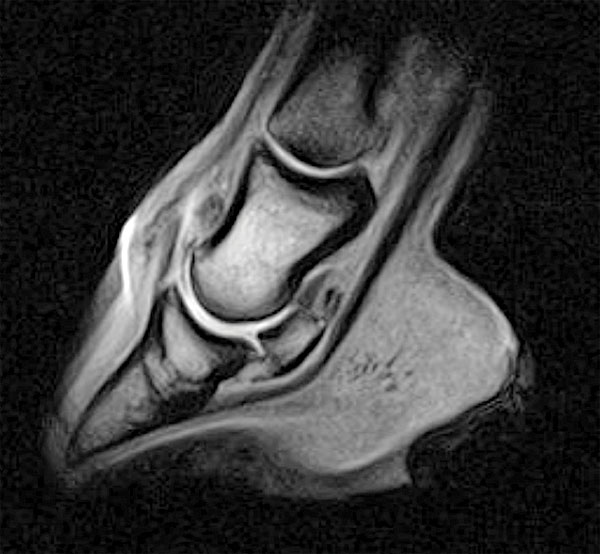
There are two options for obtaining an MRI. High-field (the magnet is very strong) MRI gives the most detailed, accurate results but requires that your horse be put under general anesthesia. Low-field (the magnet is not as strong) MRI may lack some image quality, but can be done with your horse standing and sedated, avoiding the risk of anesthesia. As equipment has improved, images of the foot obtained with low-field MRI are often good enough to provide a diagnosis.
Pros: MRI provides a very detailed, specific image of all parts of your horse’s foot. High-field MRI is the most sensitive of all of the available imaging tools, and will detect abnormalities that can’t be seen on radiographs or aren’t clear on ultrasound. MRI is the only way to identify bone edema, or fluid accumulation within the bone, that often accompanies lameness.
MRI has only been available since the late 1990s, and is often recommended for horses with a lameness that’s been isolated to the foot but shows no abnormalities on radiographs or ultrasound. Historically a last resort for horses that have responded poorly to early treatment, MRI is now recommended earlier in the lameness workup. An MRI that gives you an accurate early diagnosis can go a long way toward making good treatment and management decisions, and will improve the chances your horse will fully recover.
Cons: High-field MRI requires anesthesia, so risks must be considered if low-field MRI is unavailable or image quality is questionable. It takes a long time to create an MRI image, so it’s best if the source of lameness has been accurately located prior to imaging. MRI is best for soft-tissue injuries, and may not be as accurate as CT for identifying some bone abnormalities. MRI doesn’t allow for evaluation of blood flow.
Computed Tomography (CT Scan)
Just like radiographs, a CT scan passes radiation through your horse’s body toward a plate that then detects the amount of radiation spread through the tissues to create an image. Instead of a single beam, the CT scanner passes many small beams from different angles, creating slices of information that combine to produce a very detailed image. The X-ray tube rotates around the patient, as well as “slides” along its length, which eliminates any loss of information about a specific structure because it’s obscured by another structure. CT scans provide very detailed images of both bone and soft-tissue structures.
Pros: CT scans are much more sensitive for detecting bone lesions than radiographs, and compare favorably to low-field MRI for many soft-tissue injuries. They also allow for evaluation of blood flow, which can’t be done with MRI. It takes much less time to produce an image using CT compared with MRI, meaning larger areas are easier to evaluate and precise localization of the source of lameness isn’t as critical.
Cons: The majority of feet CT scans require anesthesia, so risks must be considered. Standing CT of the head and neck is possible, however, and work is being done to allow for standing CT scans of the feet in the near future. CT is typically not as accurate as high-field MRI for diagnosing soft-tissue injuries, and it will not identify bone edema.
Nuclear Scintigraphy (Bone Scan)
Nuclear scintigraphy involves injecting your horse with a radioactive substance that circulates throughout his bloodstream. A gamma camera creates images by detecting areas of increased radioactivity, indicating increased blood flow—a sign of inflammation.
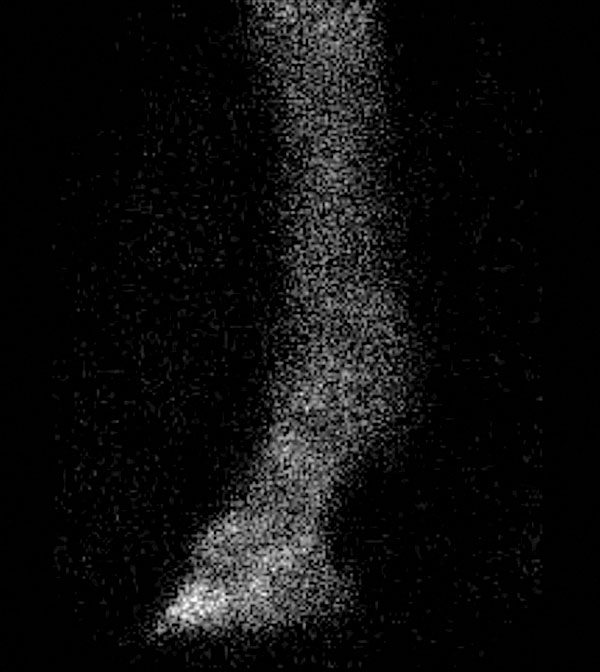
Pros: A bone scan identifies areas of active inflammation and is often combined with other imaging modalities to determine if the anatomic abnormalities identified are significant. It can be helpful for localizing a source of lameness where results from a clinical lameness exam are unclear. Bone scans can also help identify areas of subclinical inflammation—problems that are brewing but might not yet cause lameness. This allows for early management before injuries become severe.
Cons: Images obtained with a bone scan do not provide good anatomic detail. Additional imaging, including radiographs, ultrasound, MRI, or CT, are necessary to accurately diagnose the precise cause of lameness.
CASE IN POINT
Is it important to identify the cause of lameness so specifically? In some cases, absolutely! Here’s one case I encountered.

Scooter is a 14-year-old Paint mare used for breed-show-level competition. She’d shown some foot sensitivity over the years, and performs better if shod with pads. Last fall, after a hard summer of showing, she started balking. Then one day, she became very lame.
During her exam, Scooter was quite lame on the left front foot, and was uncomfortable when the lower joints of both forelimbs were flexed. With a nerve block to her left front heel and sole, Scooter became slightly lame on the right front foot. When we blocked her right front heel, she moved better than she had in years. There were no abnormalities seen on radiographs of her front feet.
Scooter improved quite a bit within a week of her sudden lameness, and her owners were given the option of treating her coffin joints with injections to reduce inflammation in many structures within the foot. If successfully treated, Scooter might be able to continue to work—and still make it to the fall shows. Alternatively, they could pursue a more specific diagnosis with an MRI.
They chose the MRI, which revealed that Scooter had edema in both navicular bones and excessive fluid in her coffin joints. The most significant finding, however, was a tear in her deep digital flexor tendon at the level of the navicular bone. In other words, she had some evidence of inflammation that most likely explained her chronic low-grade foot soreness and a significant soft-tissue injury that was most likely the cause of her acute lameness.
Scooters’s coffin joints were injected with steroids and hyaluronic acid to reduce inflammation. She was also administered Tildren, a medication that inhibits osteoclasts—cells that are involved with bone degeneration—and is especially effective for treating bone edema. After several months of rest, she was put into a very careful rehabilitation program to allow the tendon injury to heal. After a full year off, Scooter was sound and back in the competition ring.
Had Scooter’s owners taken the option of treating her coffin joints and keeping her in work, it’s likely she’d have been sound for a period of time. However, the deep digital flexor tendon injury could’ve worsened and had a significant impact on her long-term soundness. In fact, she might’ve become permanently lame. Because her owners obtained an accurate diagnosis, they were able to treat her appropriately, give her adequate time to heal, and improve the chances that their horse would stay sound for the long haul.



