Joints equal movement, and movement equals athletic performance. In fact, when it comes right down to it, muscles, tendons, and ligaments—all of the critical structures in your horse’s musculoskeletal system—are simply there to help joints move. When joints move freely and smoothly, your horse does, too. And when they don’t, troubles begin.

What’s the Scoop?
Estimates say that 60 percent of all lameness is due to osteoarthritis. It’s defined by joint disease expert Dr. Wayne McIlwraith of Colorado State University as a “progressive deterioration of the articular cartilage accompanied by changes in the bone and soft tissues of the joint.” That’s why there’s so much attention paid to discovering new techniques for accurately diagnosing and effectively treating joint disease.
In this article, we’re going to take an up-close look at your horse’s joints, including how they function and how things go wrong. Then, we’ll see how new technologies continue to improve our ability to diagnose and treat joint problems in your horse. Finally, you can refer to our comprehensive overview of treatment options.
Joint Structure
Simply put, joints are the connections between bones that allow for movement. Every joint has the same basic design made up of the following structures.
Joint capsule. A fibrous layer that encloses the entire joint, it contains blood vessels and nerves that help supply nutrients and maintain joint function. Synovial (joint) membrane. A thin layer of tissue that filters blood and produces synovial fluid.
Synovial fluid. Fluid released by cells of the synovial membrane that helps cushion the joint. It also provides nutrients to the cartilage and lubrication that facilitates joint movement.
Cartilage. A fibrous, white covering over the ends of the bones that makes up the actual gliding surface of the joint. The cartilage also has shock-absorbing properties that help distribute stresses placed on the joints during movement.
Subchondral bone. The layer of bone directly below the cartilage that helps absorb shock, and carries nutrients and waste to and from the joint.
Gone Wrong
Periarticular support structures. Tendons and ligaments surrounding the joint that help maintain stability. Most joints have a pair of collateral ligaments on the medial (inside) and lateral (outside) that provide support, in addition to various other small ligaments that contribute to the joint’s function.
Why does joint disease happen? According to Dr. McIlwraith, injuries occur either due to abnormal forces on normal cartilage, or normal forces on abnormal cartilage. In other words, a normal, healthy joint can become damaged with a sudden traumatic event such as a fall or twist in the pasture, or due to heavy repetitive use that’s commonly a part of everyday life for a hard-working performance horse. And if the cartilage in a joint is abnormal to begin with (for example, due to developmental orthopedic disease), simply strolling around the pasture can result in enough trauma to cause the joint to begin deteriorating.
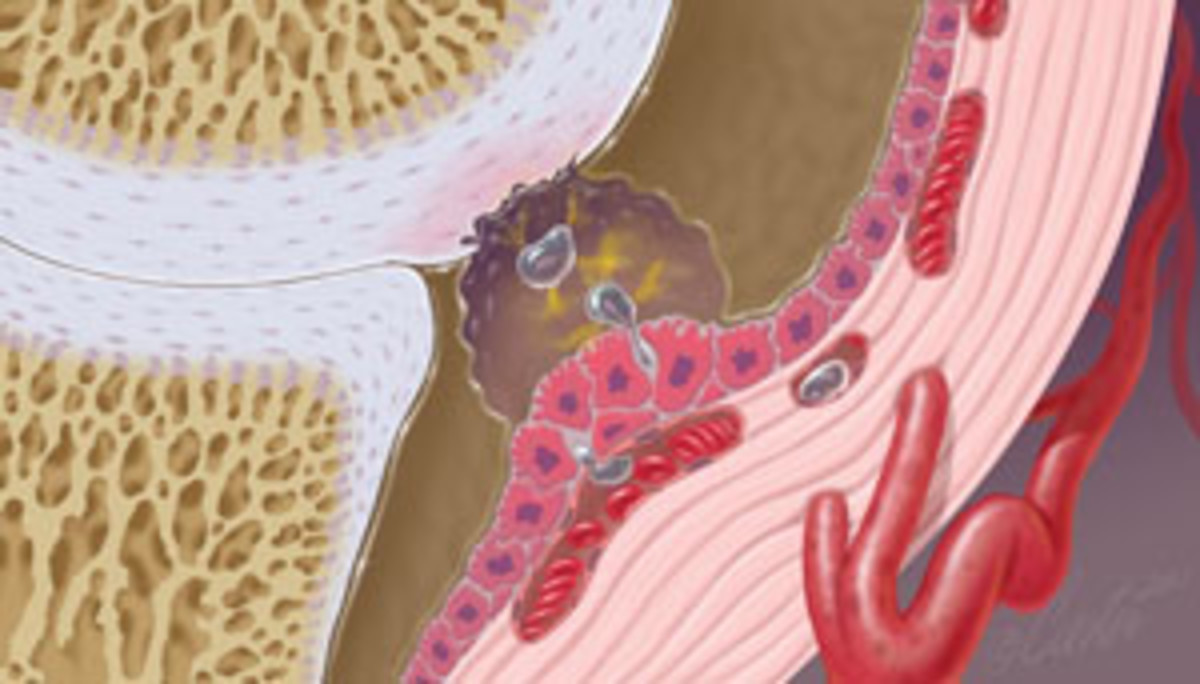
Any of the joint structures can be the first to be damaged—leading to a cascade of events that eventually involves most of the joint. Commonly, synovitis, or inflammation of the synovial lining, is the first thing that happens, often as a result of repetitive, cyclical trauma. When the synovium becomes inflamed, enzymes and other large molecules (called inflammatory mediators) are released into the synovial fluid. From the outside, you’ll see fluid accumulation (effusion) in the joint capsule that can make the joints appear swollen or enlarged. From the inside, the enzymes and other substances released wreak havoc on the surface of the cartilage, and the process of joint degeneration begins.
It’s also possible that an injury to one of the soft-tissue supporting structures of the joint can start the process of degeneration by causing instability of the joint. This results in inflammation, synovitis, and eventual cartilage breakdown. Finally, splitting and fragmentation of the cartilage or microfractures of the underlying bone can be the initial insults that begin the process. No matter how it starts, once the process of degeneration begins, it’s usually progressive over time.
Making a Diagnosis
Perhaps the most important part of diagnosing joint disease is doing it early, because early treatment can help break the cycle of degeneration and slow progression. What steps should you take.
Clinical exam. Even with more advanced diagnostic tests being made available every year, a hands-on exam of your horse may still be the most important step for making an early diagnosis. Lameness, pain with flexion, and effusion are three early signs that a joint is in danger, and mean you should take a closer look, because early treatment at this stage could help prevent long-term damage. Call your vet as soon you see any of these signs. As the disease progresses, you’ll see swelling or thickening of the joint and a decreased range of motion.
Radiographs. Radiographs are the first thing most people think of when trying to diagnose arthritis in the joints, yet they’re really most useful when damage is already severe. A radiograph won’t detect any of the early stages of joint disease, such as inflammation of the synovial lining, abnormal joint fluid, soft-tissue injuries, or inflammation of the underlying bone. Unless it’s so severe that the joint space is narrowed or cartilage defects extend to underlying bone, even cartilage damage won’t show up on radiographs in a majority of cases. Does that mean you should skip radiographs altogether? Absolutely not. Radiographs will show signs of advanced disease, and are still useful for monitoring progression in a horse with osteoarthritis.
Ultrasound. Once thought of only for diagnosing soft-tissue injuries, ultrasound of joints can now be an important part of diagnosing osteoarthritis, particularly of the stifle joint. Debris can be seen floating in the joint fluid, and thickening of the synovial lining and ligament injuries in the supporting structures also can be seen. Damaged cartilage that can’t be seen on radiographs will often be visible with an ultrasound exam. Many abnormalities can be seen with ultrasound in a joint that looks normal on a radiograph. More and more commonly, ultrasound is recommended for examination of a joint.
Nuclear scintigraphy. Scintigraphy or “bone scan” involves injection of a radioactive substance into your horse’s bloodstream that then accumulates in areas of inflammation because of increased blood flow. This can be very sensitive for detecting inflammation of the subchondral bone, a potential early sign of osteoarthritis.
Magnetic resonance imaging (MRI). MRI produces a detailed picture of all of the structures of the joint, and can be the most specific diagnostic tool for identifying joint disease at any stage of the game. MRI exams may be performed either standing or under general anesthesia. In general, standing MRI is best for examining structures from the fetlock down, where movement is less likely to be a problem, while general anesthesia will be necessary for joints above the fetlock.
Looking Forward
If early diagnosis is the key, wouldn’t it be great if a simple blood test could give evidence of early joint disease? It sure would, and recent research has identified specific substances called “biomarkers” that are detectable not only in the joint fluid, but also in the bloodstream of horses with compromised joints.
Although these tests aren’t currently available to most horse owners, they look promising in the research setting, and may someday be routinely offered by your veterinarian. Regular blood tests for biomarkers of at-risk horses could identify those with early, otherwise undetectable joint disease. Once identified, these horses could be carefully examined, and treated early—potentially halting osteoarthritis in its tracks.
Treatment Options
If 60 percent of lameness is due to joint disease, it’s easy to see why there’s so much emphasis on discovering new and more effective treatments. From the “tried and true” to the “new and cool,” a wide variety of treatment options is available. Here, I’ll name each treatment, explain how it helps, give you the benefits and downsides, and supply an estimated cost.
Systemic (oral or injectable) NSAIDS. Non-steroidal anti-inflammatories include phenylbutazone, flunixin meglumine (Banamine), and firocoxib (Equioxx). NSAIDS inhibit specific enzymes to block pathways of inflammation. This not only helps control pain and lameness, but can also minimize damage caused by inflammatory mediators released in the early stages of joint disease. NSAIDS are generally inexpensive and effective. Because they’re administered systemically, they impact multiple joints. NSAIDS can have toxic effects on the kidneys and the GI tract. Of the available choices, firocoxib is the least toxic, because it more specifically blocks one side of the inflammatory pathway, sparing substances (called prostaglandins) that can be protective. Cost is estimated between $0.50 and $15 a day, depending on the drug and form used.
Topical NSAID (diclofenamic acid, or Surpass). This anti-inflammatory cream is applied directly over the diseased joint and helps minimize damaging effects of inflammation. It’s been shown to be “disease modifying,” meaning it not only controls symptoms but also can improve the overall health of the treated joint. This treatment only affects the joint that’s treated, limiting its usefulness for horses with multiple diseased joints or when a specific diagnosis is not available. Expect to pay between $60 and $80 for a tube of cream that can treat a specific joint for two to three weeks, depending on size of the area covered.
Intra-articular corticosteroids. A corticosteroid injected directly into the joint is one of the more efficient and effective ways of controlling inflammation. By controlling inflammation, subsequent damage and progression of disease is minimized. Significant improvement in signs of pain and lameness is usually observed following injection. Contrary to popular belief, injection of steroids into a diseased joint will have no negative effect on future joint health. That said, there is risk of joint infection if proper precautions aren’t taken during the injection process, and frequent injection with high doses of some types of steroids can degrade the joint over time. A single joint injection will typically cost between $100 and $300, and will be most expensive if another substance, such as hyaluronic acid, is included in the injection.
Intra-articular hyaluronic acid (HA). HA injected directly into the joint provides lubrication and nutrition. Most commonly, HA will be injected in conjunction with a corticosteroid. HA injection can help improve overall joint health. As with steroids, direct injection into joints carries the risk for infection if proper precautions aren’t taken during the injection process. A single joint injection with HA will typically cost between $100 and $300. Similar to corticosteroids, cost will vary depending on what combination of medications is used.
Interleukin receptor antagonist protein (IRAP). For this treatment, your horse’s blood is collected and processed in order to obtain a substance that, when injected into the joint, blocks the receptors for interleukin. Interleukin is one of the most significant inflammatory mediators that causes damage in the diseased joint. Joints treated with IRAP show reduced lameness, reduced synovial inflammation, and improved cartilage health. Most experts agree that this is one of the most promising and effective joint treatments available. IRAP therapy is expensive, though, and most effective when performed early in the progression of the disease. Unfortunately, it’s often not used until later in the disease process, after other therapies have failed. There is some chance of an adverse reaction with increased heat, swelling, and pain following a second injection into a joint. Preparation of IRAP for injection can range as high as several thousand dollars, which produces enough to perform a series of two to three injections.
Intravenous hyaluronic acid (Legend). Three IV injections administered at weekly intervals are recommended to improve lubrication and nutrition to the joints. The treatment may have some anti-inflammatory effect. Because it’s administered into the bloodstream rather than directly into the joint, IV hyaluronic acid can benefit multiple joints with a single treatment. Cost is $90 to $120 per injection.
Intramuscular polysulfated glycosaminoglycan (Adequan). Seven IM injections at four-day intervals are recommended to improve cartilage health. Like Legend, Adequan is administered systemically rather than into a single joint, meaning it can benefit multiple joints with a single treatment. Because it’s administered into the muscle, it can easily be administered by most horse owners. Cost ranges from $40 to $50 per injection.
Intramuscular pentosan polysulfate. Four weekly IM injections are suggested to improve cartilage health and the quality of the synovial fluid in addition to having some anti-inflammatory effect. Like Adequan, it’s administered in the muscle, making it easy for horse owners to administer and useful for treating horses with multiple-joint involvement. Pentosan is an Australian drug that’s not FDA-approved for use in the United States, meaning it’s generally available only through compounding pharmacies. Cost is $50 to $80 per injection.
Oral joint supplements. These feed additives contain a variety of different substances, most commonly including chondroitin sulfate, glucosamine, or hyaluronic acid, that are believed to provide nutrition and protection to the joints. It can cost $100 per month or more to maintain your horse on an oral joint supplement.

