Your normally free-moving horse has been a little choppy in his striding lately. You’ve noticed shortened steps, and even an occasional head nod when you work him on a small circle. Most recently, you saw him pointing one foot, then the other, when standing tied in the barn aisle.
If you’ve been around horses for any length of time, this scenario will strike fear in your heart. The “n” word—navicular—isn’t one you want to hear, and with these symptoms, you’re sure it’s coming.
Not so fast. While it’s true the small navicular bone within your horse’s foot and its associated structures can cause a host of problems, there are also many other possible explanations for your horse’s lameness—with just as many possible treatment options. And, as any veterinarian will tell you, the most important factor for successful treatment is an accurate diagnosis.
In this article, I’ll outline all the steps that could be needed to pin down the cause of your horse’s heel pain. I’ll also describe the types of problems likely to be identified at each step along the way.
If you’re lucky, the cause of your horse’s lameness will be easy to identify early in the process. If you’re not, it can be a long and frustrating (and expensive) road to travel. One thing remains true, however: Wherever you end up, your odds for success increase with a treatment plan that targets the actual cause. (Note: For those of you on a strict veterinary budget, I’ll also outline alternative management plans to help you play the odds while minimizing risk.)
Step 1: The Clinical Exam
This is probably the most important part of making an accurate diagnosis, because even the most high-tech diagnostic tests usually mean nothing without a thorough physical exam.
During a clinical lameness exam, your vet will:
• palpate and manipulate your horse’s legs and body and apply hoof testers to his feet;
• watch your horse walking and trotting in hand, plus working on the longe line and under saddle;
• perform flexion or stress tests on the joints; and
• probably recommend doing diagnostic blocks (anesthetic placed into nerves or fluid structures) to help pinpoint the precise source of your horse’s lameness.
What you’ll learn: Whether the pain your horse is experiencing originates from his heels, and whether one or both feet are involved. If both feet are sore, the odds increase that your horse has a bone- or joint-related problem—and classic “navicular syndrome” is on that list of possibilities. If only one foot hurts, your vet might wonder about a soft-tissue injury, such as a small ligament tear, particularly if your horse’s lameness is acute (sudden onset).
Approximate cost: Up to $300, depending on the clinician and number and type of diagnostic blocks performed.
Now what? In most cases, the recommended next step would be radiographs of your horse’s feet. Ideally, you’d have these done before pursuing any treatment options.
The economy plan: During the clinical examination, your vet might identify shoeing or trimming imbalances that could be corrected, or simply suggest some corrective measure that could make your horse more comfortable. Some horses with heel pain will benefit from shoeing strategies that provide better heel support or ease the stress of breakover (such as egg-bar shoes with a rocker toe and/or some type of pour-in pad). Corrective shoeing with some carefully administered non-steroidal anti-inflammatory medications could be enough to help your horse. If he’s still lame after that, however, you should save your pennies for some pictures of his feet.
Step 2: Radiographs
Radiographs (x-rays) of your horse’s feet provide a picture of the pastern, coffin, and navicular bones as well as of the coffin joint. For best-quality radiographs, your horse’s shoes should be pulled. Your vet will typically take between three and five different views of each foot.

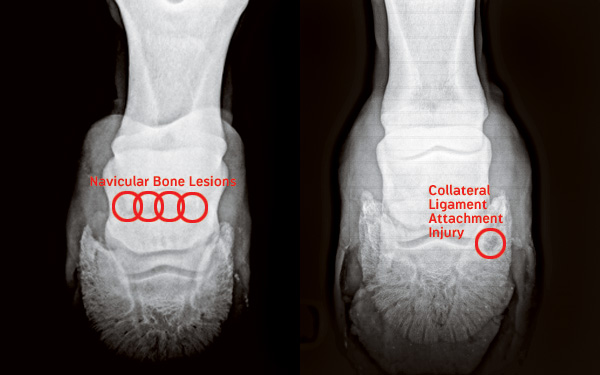
What you’ll learn: Whether there are abnormalities in your horse’s navicular bone, coffin bone, or coffin joint. In addition, your vet might be able to detect problems at points where soft-tissue structures attach to bone. Radiographs are also the most accurate way to identify hoof-balance issues, plus they can provide a lot of information about ideal corrective shoeing.
Approximate cost: With new digital radiology systems, expect to pay approximately $40 per view, or between $250 and $400 for a full set of high-quality foot radiographs.
Now what? Specific shoeing recommendations can come from radiographs. If navicular-bone changes are identified as a likely underlying cause of your horse’s lameness, your vet might recommend injection of the coffin joint and/or navicular bursa (the fluid structure between the navicular bone and the deep digital flexor tendon where it runs beneath the foot) with hyaluronic acid and corticosteroids. If these joint injections solve your horse’s problem for an extended period of time (say, six to 12 months), your vet might recommend repeating them as needed to help keep your horse sound.
Additional treatment with systemic joint medications such as Adequan® or Legend®, plus intermittent use of NSAIDs, could also be part of your long-term management plan.
Finally, if there appears to be significant degeneration of the navicular bone, Tildren® might be suggested as a treatment option. (See the treatment guide on the next page for specific information about these different therapies.)
If no explanation for your horse’s lameness is apparent on radiographs, ultrasound might be recommended—especially if your vet suspects a soft-tissue injury or if your horse doesn’t respond well to initial therapy.
The economy plan: If nothing shows on the radiographs and your vet suspects a soft-tissue injury but you just can’t afford to ultrasound, he or she might still suggest joint injections—along with an extended period of rest and rehabilitation (six to 12 months). The corticosteroids will help quiet inflammation and can be beneficial, but if a soft-tissue structure is an underlying cause, then the rest is critical as well. (You could cause greater damage if you continue to work your horse.)
Step 3: Ultrasound
Ultrasound captures images of soft-tissue structures by passing sound waves through tissues to produce a picture. A number of common foot-related soft-tissue injuries can become apparent with ultrasound, although the hoof wall makes visualization of some structures more difficult.
What you’ll learn: Whether there are soft-tissue injuries, such as tears in the:
• collateral ligaments of the coffin joint;
• deep digital flexor tendon where it runs beneath the foot; or
• small impar ligament that attaches to the bottom of the navicular bone.
Approximate cost: Typically between $150 and $400, depending on the clinician and equipment used.
Now what? If a specific soft-tissue injury is identified, it could be possible to treat the area with injections such as platelet-rich plasma or stem cells. Shockwave therapy, to help stimulate healing, might be recommended as well. Your vet can also map out suitable rest and rehabilitation plans, plus monitor healing with follow-up ultrasound exams.
If no soft-tissue injuries show up, or if your vet questions the significance of what is seen, the next diagnostic step will either be a bone scan or an MRI.
The economy plan: Ultrasound marks the end of the diagnostic road for many horse owners because of the high cost of additional tests. If you still don’t have a specific diagnosis but just can’t spend another dime, it’s best to play it safe and assume there’s a soft-tissue injury somewhere within your horse’s foot. Again, your vet might recommend joint and/or bursa injections, and extended rest is critical to avoid further damage.
Step 4: Bone Scan
Your horse will be administered an intravenous dose of a radioactive substance that circulates throughout his bloodstream. A specialized camera detects areas of increased radioactivity within your horse’s body, indicating the increased blood flow that’s associated with inflammation.
What you’ll learn: Where areas of active bone inflammation are—even if there’s nothing obvious on radiographs. It’s especially useful for identifying injuries where tendons and ligaments attach to bone—such as at the attachment of the deep digital flexor tendon to the bottom of the coffin bone.
Approximate cost: $800 to $1,200 for evaluation of the feet alone.
Now what? If the bone scan provides a specific answer, your vet can target appropriate therapy to your horse’s problem. For example, stem cells and shockwave therapy might be suggested for a specific soft-tissue injury, or joint injections and Tildren could be suggested for a degenerative bone problem.
The economy plan: None.
Step 5: Magnetic Resonance Imaging
MRI produces an extremely detailed image of both bone and soft-tissue structures through the use of a strong magnetic field that detects radio waves emitted from the body. MRI units are available for imaging your horse while standing and sedated, although better images can generally be obtained under anesthesia.
What you’ll learn: Precisely what the relevant bones and soft tissues look like. MRI is especially useful for identifying injuries of the small soft-tissue structures within the foot and is the diagnostic tool most likely to yield a specific diagnosis.
Approximate cost: $1,500 to $2,000.
Now what? Once again, a specific diagnosis will allow your vet to come up with a treatment plan most likely to be successful for your horse’s future soundness.
The economy plan: None.






